In honor of National Public Health Week 2023
Written by Alexis Wing
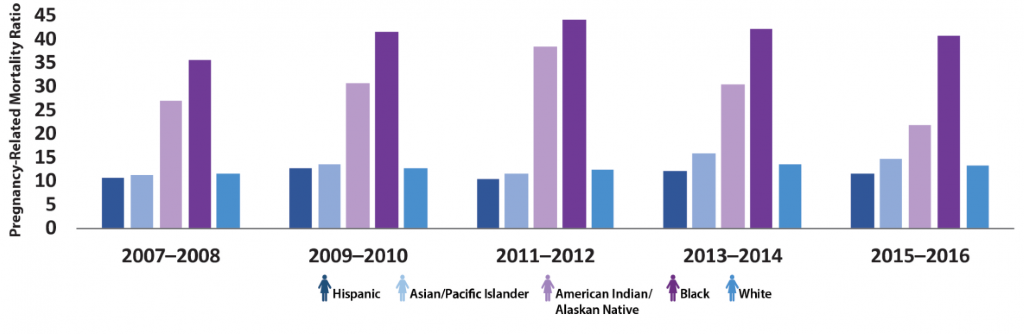
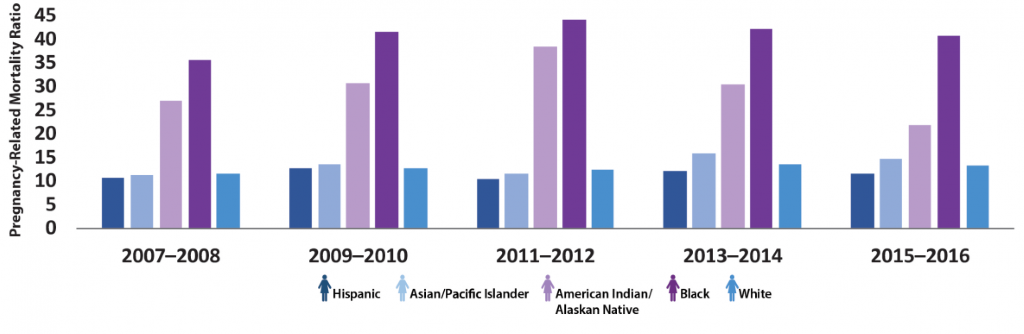
While inequities based on race and ethnicity manifest across different sectors of society such as education, socio-economic status, and housing, they are especially apparent as health inequities, exemplified by the domain of maternal and child health. The United States has the highest maternal mortality rate among all developed nations, but the risk of maternal mortality or a pregnancy associated death for black women is 3 to 4 times higher than for white women. This demonstrates how racism is both a social justice and public health issue, as it negatively impacts the health of black women on a structural and systemic level. Pregnancy-related mortality ratios by race, 2007-2016
When we talk about the barriers to achieving equitable maternal health, it is imperative to not only discuss maternal mortality, but to broaden this conversation to include pregnancy-associated mortality and severe maternal morbidity (SMM) as well. Pregnancy associated mortality includes maternal deaths that occur within 1 year of the pregnancy and SMM takes into account the negative long-term impacts that pregnancy complications can have on a woman’s health. According to the CDC, blood transfusions (typically given in response to excessive bleeding during delivery) account for the greatest percentage of women with SMM. This also disproportionately affects women of color, as black non-Hispanic women are twice as likely to experience SMM as compared with white non-Hispanic women. These disparities in pregnancy associated mortality and SMM persist in our communities in Massachusetts as well. Black non-Hispanic women in the state are twice as likely to experience pregnancy associated mortality compared to white non-Hispanic women. We need to consider both pregnancy associated mortality and severe maternal morbidity when we collect or look at data, as broadening this focus allows us to have a more holistic view of the community and thus identify and understand the barriers to equitable maternal health.
We need to understand that the injustices faced by black women across the country, and in Massachusetts specifically, are attributed to a number of complex factors. These include (but are not limited to) structural and institutional racism, implicit biases in health care, disparities in access to adequate prenatal care, and the inequitable allocation of resources from government structures. It is essential for community coalitions and organizers to advocate for more equitable research, policies, and practices to improve maternal health throughout the state.
For example, a bill to reduce racial disparities in maternal health was introduced to the state legislature a little over a year ago and is expected to pass later this year. It aims to investigate many of these complex factors, with a specific focus on community-driven strategies to address these disparities. While supporting legislation like this is important to achieving equity, community coalitions can also play a role in seeing through and supporting the equitable implementation of the activities and allocation of resources outlined in these bills.

In the process of working towards equitable maternal and child health, it is also important to consider women struggling with substance use addiction. Although Massachusetts has historically seen a lower pregnancy associated mortality rate than what is experienced on a nationwide level, there was an alarming 33% increase between 2012 and 2014. Consequently, the Massachusetts Maternal Mortality and Morbidity Review (MMMMR) Committee launched an inquiry to investigate potential contributing factors. They found that of the 199 pregnancy-associated deaths in Massachusetts that occurred between 2005 and 2014, approximately 1 in 5 were related to substance use. This aligns with the increase in opioid overdose deaths in Massachusetts during the same time period, as the total number of opioid deaths have increased fivefold in the state over the last 20 years. Pregnant women were not spared from this opioid crisis, as over one third of deaths among women delivering a live birth between 2011 and 2015 were fatal opioid-related overdoses. Pervasive stigma against people who use drugs, and especially women who use drugs, is an upstream factor that contributes to these maternal health inequities. Community coalitions can take action to address them by combating stigma in their communities through education, awareness, and advocacy. Although both stigma against women who use substances and racism are factors that perpetuate serious health inequities, they do so in different ways and should not be treated as equivalent to one another. However, these issues can and do intersect in the realm of maternal health and it is important for coalitions to consider intersectional strategies to address the health inequities they cause.

Even though this data may feel overwhelming, there are actions that community coalitions can take to improve care for pregnant women struggling with substance use disorder (SUD). One comprehensive effort to address the disparity in maternal health care for women with SUD is the Maternal Opioid Use During Pregnancy Toolkit developed by the Massachusetts Perinatal Quality Collaborative. The development of this toolkit was a product of collaborative effort that brought together groups with multi-disciplinary expertise. The toolkit itself contains a vast range of resources to support and identify the special treatment needs of women with SUD during pregnancy and postpartum. It also emphasizes the importance of cross-disciplinary partnerships in this work and comprehensive care integration to address the unique needs of pregnancy that are concurrent with SUD. Community coalitions can also consider taking a similar approach by advocating for a more integrated model of care that simultaneously addresses issues related to SUD and maternal health. Although the disparities facing black women and women with SUD in maternal health can seem daunting, it is important to remember that moving towards equitable policies and practices is a process, and that even small steps taken in the community to address them can have a significant impact on the health of one person or one family.
Further Reading:
Racial Disparities in Maternal Health
Why Black Women Face More Health Risks Before, During, and After Pregnancy
Massachusetts Maternal Mortality Rates: Opioid Abuse and Psychiatric Illness Play a Role